Health
WHO declares monkeypox Public Health Emergency
“There’s clear risk of further international spread, although the risk of interference with international traffic remains low for the moment”

The World Health Organization’s Director-General Dr. Tedros Adhanom Ghebreyesus declared the escalating global monkeypox outbreak a Public Health Emergency of International Concern (PHEIC) on Saturday. This is an escalated status but below the requirements needed for a declaration of a pandemic, in part over its low death rates.
Currently, the vast majority of reported cases are in the WHO European Region. “WHO/Europe remains committed to partnering with countries and communities to address the outbreak with the required urgency,” Dr. Tedros said during a media briefing.
In laying out reasons for the declaration the WHO head noted; “We have an outbreak that has spread around the world rapidly through new modes of transmission, about which we understand too little,” Tedros said. “I know this has not been an easy or straightforward process and that there are divergent views.”
There had been reservations by the health agency’s expert committee who said the monkeypox outbreak did not yet amount to an international emergency in a meeting in June. Tedros had reconvened that committee in a special session this past Thursday.
“A month ago, I convened the Emergency Committee under the International Health Regulations to assess whether the multi-country monkeypox outbreak represented a public health emergency of international concern,” Tedros told reporters. “At that meeting, while differing views were expressed, the committee resolved by consensus that the outbreak did not represent a public health emergency of international concern.”
“At the time, 3040 cases of monkeypox had been reported to WHO, from 47 countries. Since then, the outbreak has continued to grow, and there are now more than 16 thousand reported cases from 75 countries and territories, and five deaths,” he added.
“In light of the evolving outbreak, I reconvened the committee on Thursday of this week to review the latest data and advise me accordingly. I thank the committee for its careful consideration of the evidence, and issues,” Tedros continued.
“On this occasion, the committee was unable to reach a consensus on whether the outbreak represents a public health emergency of international concern. The reasons the committee members gave for & against are laid out in the report we are publishing today.”
“Under the International Health Regulations, I am required to consider five elements in deciding whether an outbreak constitutes a public health emergency of international concern.”
“First, the information provided by countries – which in this case shows that this virus has spread rapidly to many countries that have not seen it before. Second, the three criteria for declaring a public health emergency of international concern under the International Health Regulations, which have been met. Third, the advice of the Emergency Committee, which has not reached consensus. Fourth, scientific principles, evidence and other relevant information – which are currently insufficient and leave us with many unknowns. Fifth, the risk to human health, international spread and the potential for interference with international traffic,” Tedros told the press laying out the foundation to his decision.
“WHO’s assessment is that the risk of monkeypox is moderate globally and in all regions, except in the European region where we assess the risk as high,” he said adding “There is also a clear risk of further international spread, although the risk of interference with international traffic remains low for the moment.”
“So in short, we have an outbreak that has spread around the world rapidly, through new modes of transmission, about which we understand too little and which meets the criteria in the International Health Regulations.” The WHO chief then noted “For all of these reasons, I have decided that the global monkeypox outbreak represents a public health emergency of international concern.”

(Photo credit: WHO)
Tedros then pivoted to WHO recommendations for the international public health community in addressing the outbreak.
“Accordingly, I have made a set of recommendations for four groups of countries: First [group], those that have not yet reported a case of monkeypox, or have not reported a case for more than 21 days. Second [group], those with recently imported cases of monkeypox and that are experiencing human-to-human transmission. This includes recommendations to implement a coordinated response to stop transmission and protect vulnerable groups; to engage & protect affected communities; To intensify surveillance & public health measures; To strengthen clinical management & infection prevention & control in hospitals & clinics to accelerate research into the use of vaccines, therapeutics & other tools; And recommendations on international travel. The third group of countries is those with transmission of monkeypox from animals to humans and the fourth is countries with manufacturing capacity for vaccines and therapeutics.”
Tedros acknowledged the work of the committee saying: “I thank the Emergency Committee for its deliberations and advice. I know this has not been an easy or straightforward process, and that there are divergent views among the members. “The International Health Regulations remains a vital tool for responding to the international spread of disease. But this process demonstrates once again that this vital tool needs to be sharpened to make it more effective.”
“Although I am declaring a public health emergency of international concern, for the moment this is an outbreak that is concentrated among men who have sex with men, especially those with multiple sexual partners,” he said. “That means that this is an outbreak that can be stopped with the right strategies in the right groups.”
“It’s therefore essential that all countries work closely with communities of men who have sex with men, to design & deliver effective information & services, and to adopt measures that protect both the health, human rights & dignity of affected communities,” Tedros said and then warned, “”Stigma and discrimination can be as dangerous as any virus.”
The WHO Director-General’s full statement is linked here: (WHO)
The Centers for Disease Control and Prevention released a statement saying that the agency was “supportive” of WHO’s emergency declaration and hoped it would galvanize international action to stamp out the outbreaks. The U.S. has reported more than 2,800 monkeypox cases and sent more than 370,000 vaccine doses to U.S. states reporting cases.
Speaking with reporters Friday, Jennifer McQuiston the Deputy Director for High Consequence Pathogens and Pathology at the Centers for Disease Control and Prevention said that two cases of the monkeypox virus have been diagnosed in children.
“We became aware of these cases just this week, and we’ve been working with the jurisdictions to understand more about these cases,” McQuiston said.
In a Washington Post Live session Friday, CDC Director Walensky, while discussing the highly contagious Omicron BA.5 coronavirus variant and the ongoing monkeypox outbreak, noted that the CDC was made aware of the cases adding that both children “are doing well.”
McQuiston said that the agency determined that both cases were “likely the result of household transmission” and “had no contact with each other.”
The agency is now aware of at least eight cases in people who identify as cisgender women, McQuiston said. Most cases so far have been among men who have sex with men. The number of cases as of July 22 is a total of 2,891 in the U.S. in 44 states and territories including the District of Columbia.
“There is no evidence to date that we’re seeing this virus spread outside of those populations to any degree, and I think that the primary drivers for this infection in the U.S. remain in the gay, bisexual, and men who have sex with men communities right now,” McQuiston added.
Monkeypox
US contributes more than $90 million to fight mpox outbreak in Africa
WHO and Africa CDC has declared a public health emergency
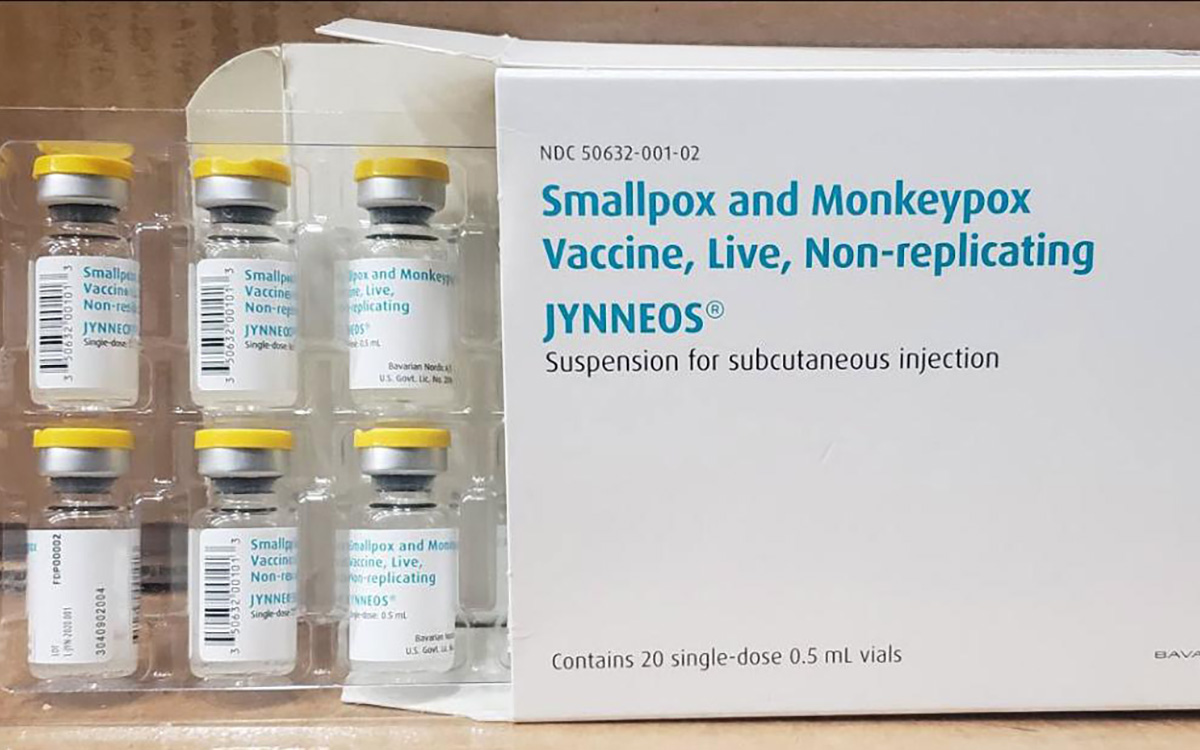
The U.S. has contributed more than $90 million to the fight against the mpox outbreak in Africa.
The U.S. Agency for International Development on Tuesday in a press release announced “up to an additional” $35 million “in emergency health assistance to bolster response efforts for the clade I mpox outbreak in Central and Eastern Africa, pending congressional notification.” The press release notes the Biden-Harris administration previously pledged more than $55 million to fight the outbreak in Congo and other African countries.
“The additional assistance announced today will enable USAID to continue working closely with affected countries, as well as regional and global health partners, to expand support and reduce the impact of this outbreak as it continues to evolve,” it reads. “USAID support includes assistance with surveillance, diagnostics, risk communication and community engagement, infection prevention and control, case management, and vaccination planning and coordination.”
The World Health Organization and the Africa Centers for Disease Control and Prevention last week declared the outbreak a public health emergency.
The Washington Blade last week reported there are more than 17,000 suspected mpox cases across in Congo, Uganda, Kenya, Rwanda, and other African countries. The outbreak has claimed more than 500 lives, mostly in Congo.
Health
Mpox outbreak in Africa declared global health emergency
ONE: 10 million vaccine doses needed on the continent

Medical facilities that provide treatment to gay and bisexual men in some East African countries are already collaborating with them to prevent the spread of a new wave of mpox cases after the World Health Organization on Wednesday declared a global health emergency.
The collaboration, both in Uganda and Kenya, comes amid WHO’s latest report released on Aug. 12, which reveals that nine out of every 10 reported mpox cases are men with sex as the most common cause of infection.
The global mpox outbreak report — based on data that national authorities collected between January 2022 and June of this year — notes 87,189 of the 90,410 reported cases were men. Ninety-six percent of whom were infected through sex.
Sexual contact as the leading mode of transmission accounted for 19,102 of 22,802 cases, followed by non-sexual person-to-person contact. Genital rash was the most common symptom, followed by fever and systemic rash.
The WHO report states the pattern of mpox virus transmission has persisted over the last six months, with 97 percent of new cases reporting sexual contact through oral, vaginal, or anal sex with infected people.
“Sexual transmission has been recorded in the Democratic Republic of Congo among sex workers and men who have sex with men,” the report reads. “Among cases exposed through sexual contact in the Democratic Republic of the Congo, some individuals present only with genital lesions, rather than the more typical extensive rash associated with the virus.”
The growing mpox cases, which are now more than 2,800 reported cases in at least 13 African countries that include Kenya, Uganda, Rwanda, and prompted the Africa Centers for Disease Control and Prevention this week to declare the disease a public health emergency for resource mobilization on the continent to tackle it.
“Africa has long been on the frontlines in the fight against infectious diseases, often with limited resources,” said Africa CDC Director General Jean Kaseya. “The battle against Mpox demands a global response. We need your support, expertise, and solidarity. The world cannot afford to turn a blind eye to this crisis.”
The disease has so far claimed more than 500 lives, mostly in Congo, even as the Africa CDC notes suspected mpox cases across the continent have surged past 17,000, compared to 7,146 cases in 2022 and 14,957 cases last year.
“This is just the tip of the iceberg when we consider the many weaknesses in surveillance, laboratory testing, and contact tracing,” Kaseya said.
WHO, led by Director General Tedros Adhanom Ghebreyesus, also followed the Africa CDC’s move by declaring the mpox outbreak a public health emergency of international concern.
The latest WHO report reveals that men, including those who identify as gay and bisexual, constitute most mpox cases in Kenya and Uganda. The two countries have recorded their first cases, and has put queer rights organizations and health care centers that treat the LGBTQ community on high alert.
The Uganda Minority Shelters Consortium, for example, confirmed to the Washington Blade that the collaboration with health service providers to prevent the spread of mpox among gay and bisexual men is “nascent and uneven.”
“While some community-led health service providers such as Ark Wellness Clinic, Children of the Sun Clinic, Ice Breakers Uganda Clinic, and Happy Family Youth Clinic, have demonstrated commendable efforts, widespread collaboration on mpox prevention remains a significant gap,” UMSC Coordinator John Grace stated. “This is particularly evident when compared to the response to the previous Red Eyes outbreak within the LGBT community.”
Grace noted that as of Wednesday, there were no known queer-friendly health service providers to offer mpox vaccinations to men who have sex with men. He called for health care centers to provide inclusive services and a more coordinated approach.
Although Grace pointed out the fear of discrimination — and particularly Uganda’s Anti-Homosexuality Act — remains a big barrier to mpox prevention through testing, vaccination, and treatment among queer people, he confirmed no mpox cases have been reported among the LGBTQ community.
Uganda so far has reported two mpox cases — refugees who had travelled from Congo.
“We are for the most part encouraging safer sex practices even after potential future vaccinations are conducted as it can also be spread through bodily fluids like saliva and sweat,” Grace said.
Grace also noted that raising awareness about mpox among the queer community and seeking treatment when infected remains a challenge due to the historical and ongoing homophobic stigma and that more comprehensive and reliable advocacy is needed. He said Grindr and other digital platforms have been crucial in raising awareness.
The declarations of mpox as a global health emergency have already attracted demand for global leaders to support African countries to swiftly obtain the necessary vaccines and diagnostics.
“History shows we must act quickly and decisively when a public health emergency strikes. The current Mpox outbreak in Africa is one such emergency,” said ONE Global Health Senior Policy Director Jenny Ottenhoff.
ONE is a global, nonpartisan organization that advocates for the investments needed to create economic opportunities and healthier lives in Africa.
Ottenhoff warned failure to support the African countries with medical supplies needed to tackle mpox would leave the continent defenseless against the virus.
To ensure that African countries are adequately supported, ONE wants governments and pharmaceutical companies to urgently increase the provision of mpox vaccines so that the most affected African countries have affordable access to them. It also notes 10 million vaccine doses are currently needed to control the mpox outbreak in Africa, yet the continent has only 200,000 doses.
The Blade has reached out to Ishtar MSM, a community-based healthcare center in Nairobi, Kenya, that offers to service to gay and bisexual men, about their response to the mpox outbreak.
Health
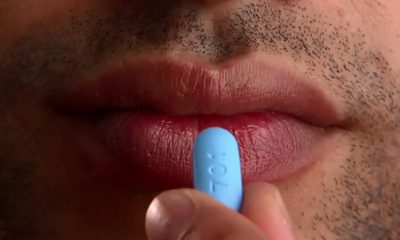
White House urged to expand PrEP coverage for injectable form
HIV/AIDS service organizations made call on Wednesday
A coalition of 63 organizations dedicated to ending HIV called on the Biden-Harris administration on Wednesday to require insurers to cover long-acting pre-exposure prophylaxis (PrEP) without cost-sharing.
In a letter to Chiquita Brooks-LaSure, administrator of the Centers for Medicare and Medicaid Services, the groups emphasized the need for broad and equitable access to PrEP free of insurance barriers.
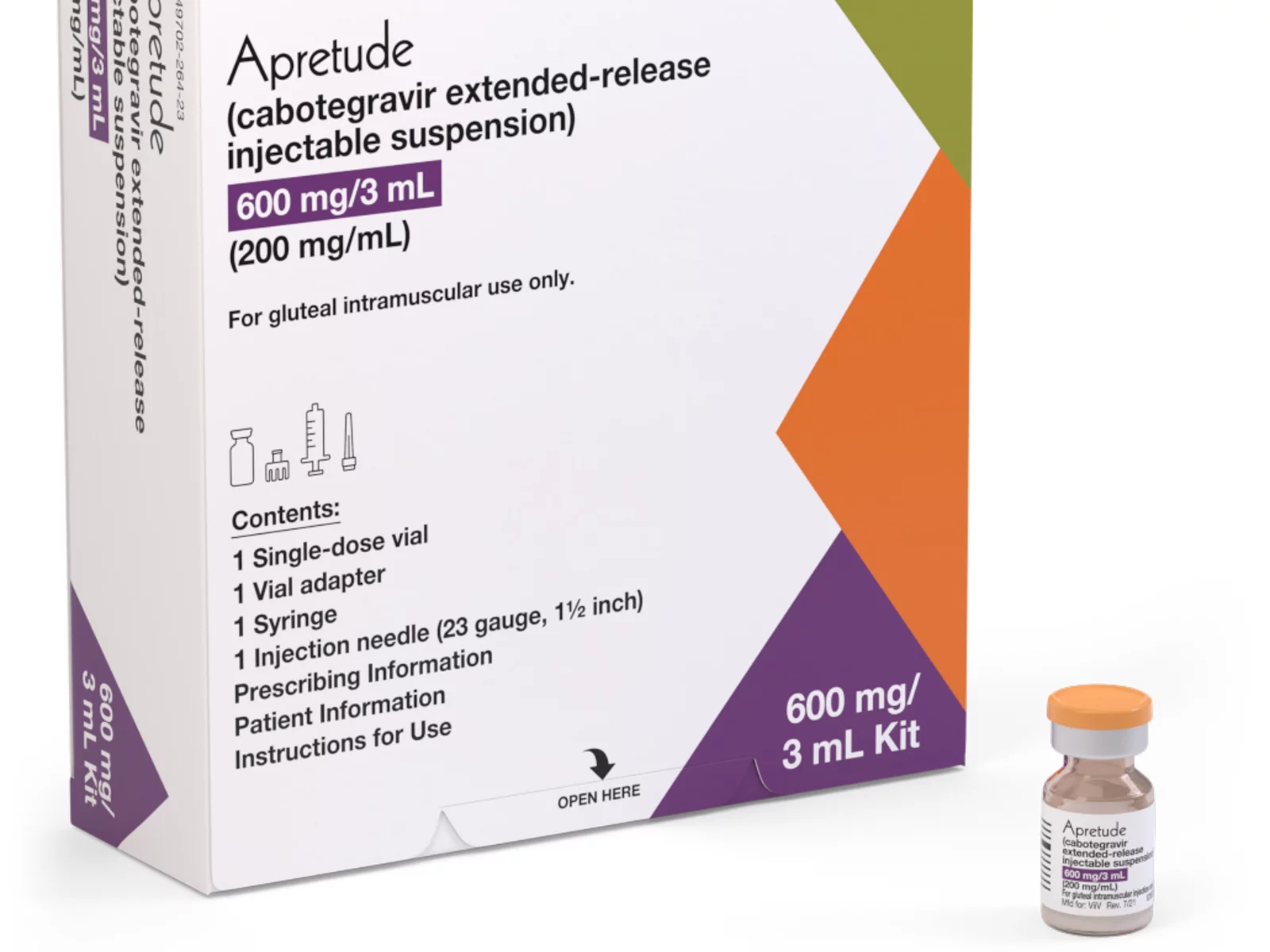
Long-acting PrEP is an injectable form of PrEP that’s effective over a long period of time. The FDA approved Apretude (cabotegravir extended-release injectable suspension) as the first and only long-acting injectable PrEP in late 2021. It’s intended for adults and adolescents weighing at least 77 lbs. who are at risk for HIV through sex.
The U.S. Preventive Services Task Force updated its recommendation for PrEP on Aug. 22, 2023, to include new medications such as the first long-acting PrEP drug. The coalition wants CMS to issue guidance requiring insurers to cover all forms of PrEP, including current and future FDA-approved drugs.
“Long-acting PrEP can be the answer to low PrEP uptake, particularly in communities not using PrEP today,” said Carl Schmid, executive director of the HIV+Hepatitis Policy Institute. “The Biden administration has an opportunity to ensure that people with private insurance can access PrEP now and into the future, free of any cost-sharing, with properly worded guidance to insurers.”
Currently, only 36 percent of those who could benefit from PrEP are using it. Significant disparities exist among racial and ethnic groups. Black people constitute 39 percent of new HIV diagnoses but only 14 percent of PrEP users, while Latinos represent 31 percent of new diagnoses but only 18 percent of PrEP users. In contrast, white people represent 24 percent of HIV diagnoses but 64 percent of PrEP users.
The groups also want CMS to prohibit insurers from employing prior authorization for PrEP, citing it as a significant barrier to access. Several states, including New York and California, already prohibit prior authorization for PrEP.
Modeling conducted for HIV+Hep, based on clinical trials of a once every 2-month injection, suggests that 87 percent more HIV cases would be averted compared to daily oral PrEP, with $4.25 billion in averted healthcare costs over 10 years.
Despite guidance issued to insurers in July 2021, PrEP users continue to report being charged cost-sharing for both the drug and ancillary services. A recent review of claims data found that 36 percent of PrEP users were charged for their drugs, and even 31 percent of those using generic PrEP faced cost-sharing.
The coalition’s letter follows a more detailed communication sent by HIV+Hepatitis Policy Institute to the Biden administration on July 2.
Signatories to the community letter include Advocates for Youth, AIDS United, Equality California, Fenway Health, Human Rights Campaign, and the National Coalition of STD Directors, among others.
-

 State Department4 days ago
State Department4 days agoHIV/AIDS activists protest at State Department, demand full PEPFAR funding restoration
-

 Brazil4 days ago
Brazil4 days agoUS lists transgender Brazilian congresswoman’s gender as ‘male’ on visa
-

 Federal Government5 days ago
Federal Government5 days agoWhite House sues Maine for refusing to comply with trans athlete ban
-

 District of Columbia4 days ago
District of Columbia4 days agoCapital Pride wins $900,000 D.C. grant to support WorldPride